The Complete Guide to Dental Instruments: Essential Tools Every Practice Needs in 2026
Dental instruments are the foundation of any dental practice, enabling clinicians to diagnose, treat, and care for patients reliably. In 2026, instrument design and materials continue to evolve, improving function, comfort, and durability. This guide breaks down the main types of dental instruments, how each is used, and best practices for care and sterilization. Knowing your instruments—and choosing the right kits—directly affects efficiency, safety, and patient outcomes.
Key Takeaways
- Dental instruments remain central to safe, effective patient care and streamlined workflows in 2026.
- Core hand instruments include mouth mirrors, explorers (probes), scalers, curettes, and high-speed handpieces.
- Scalers are for supragingival calculus; curettes are shaped for subgingival cleaning and periodontal pockets.
- Forceps—both extracting and articulating types—are essential for extractions and precise tissue handling.
- Specialized instrument kits give practices the right tools for specific procedures, saving time and minimizing errors.
- Strict sterilization and routine maintenance protect patients and extend instrument life.
- Ergonomic handles and material advances reduce clinician fatigue and boost precision.
- Modern stainless steel alloys and surface treatments increase wear resistance and corrosion protection.
What Are the Key Types of Dental Hand Instruments Every Practice Needs?
Dental hand instruments form the practical toolkit for everyday exams and procedures. The essential types every practice should have on hand include:
- Mouth Mirror: Provides indirect vision and reflects light into the oral cavity for thorough exams.
- Explorer (Probe): A fine, pointed instrument used to locate caries, margins, and other irregularities.
- Scaler: Built to remove supragingival plaque and calculus from tooth surfaces.
- Curette: Designed for subgingival debridement and cleaning periodontal pockets.
- High-Speed Handpiece: The primary rotary instrument for cutting and shaping tooth structure during restorative work.
Choosing and maintaining these instruments correctly ensures clinicians can perform exams and treatments efficiently and with predictable results.
| Instrument Type | Function | Importance |
|---|---|---|
| Mouth Mirror | Provides indirect vision and illumination | Essential for full-mouth examinations |
| Explorer | Detects caries and surface irregularities | Critical for accurate diagnosis |
| Scaler | Removes supragingival plaque and calculus | Key to routine hygiene and prophylaxis |
| Curette | Performs subgingival scaling and root planing | Important for periodontal therapy |
| High-Speed Handpiece | Prepares and shapes tooth structure | Necessary for restorative and surgical procedures |
Select instruments based on the procedures you perform most often and the ergonomic needs of your team.
How Do Dental Scalers and Curettes Differ in Function and Use?
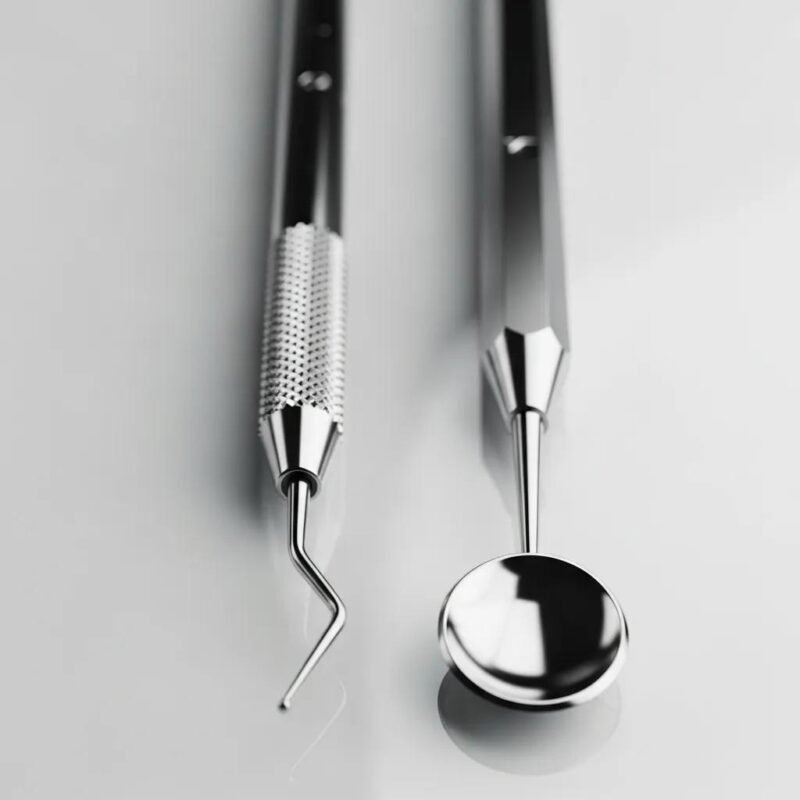
Scalers and curettes both remove deposits from teeth, but each targets different areas and requires a distinct technique.
Scalers are optimized for supragingival cleaning—scraping calculus and plaque above the gum line. They usually have pointed tips and stiff cutting edges for efficient removal on crowns and interproximal surfaces.
Curettes are intended for subgingival work. With rounded, spoon-like tips, they are gentler on soft tissue and better suited for root planing and removing deposits within periodontal pockets.
Understanding these differences helps clinicians choose the right tool for safe, thorough periodontal care.
What Are the Common Types of Dental Forceps and Their Applications?
Dental forceps are precision instruments used primarily in extractions and for handling tissues or materials. Common varieties include:
- Extracting Forceps: Engineered to grip and remove teeth—styles vary by tooth anatomy and quadrant.
- Articulating Forceps: Used to hold materials or manipulate soft tissue with controlled pressure.
- Endodontic File Holder Forceps: Provide secure handling of endodontic files and small instruments during root canal procedures.
Using the correct forceps for each task improves procedural safety and outcomes.
Which Dental Instrument Kits Are Best Suited for Different Dental Specialties?
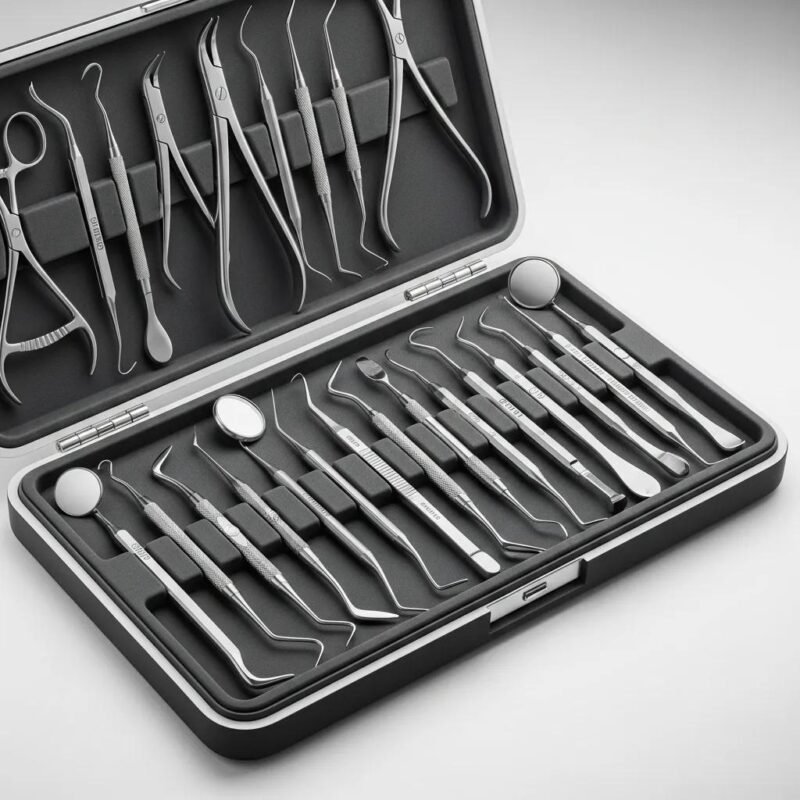
Instrument kits are built to match the needs of specific specialties. A general dentistry kit covers routine exams and restorations, while periodontics, endodontics, and oral surgery kits include specialty instruments tailored to those workflows.
Specialty kits offer clear benefits:
- Comprehensive Coverage: Kits are configured to include the instruments required for common procedures in that specialty.
- Cost-Effectiveness: Bundled purchases often reduce per-instrument cost compared with buying individually.
- Improved Efficiency: Organized kits reduce setup time and help teams maintain consistent instrument sets.
Choosing the right kit helps standardize care and keeps procedures running smoothly.
How Do Specialized Instrument Kits Improve Practice Efficiency?
Specialized kits reduce time spent gathering instruments and ensure clinicians have the exact tools required for each procedure. That organization minimizes interruptions, shortens turnover time, and lowers the chance of missing instruments during cases.
Because kits reflect specialty workflows, they also support clinical consistency and can simplify training for new staff—allowing teams to focus on patient care rather than instrument logistics.
What Should You Consider When Selecting a Dental Instrument Kit?
When evaluating instrument kits, consider these priorities:
- Quality of Materials: Durable alloys and reliable finishes extend service life and performance.
- Ergonomic Design: Comfortable grips and balanced weight reduce clinician fatigue.
- Cost-Effectiveness: Assess long-term value, warranty options, and service support alongside upfront price.
Balancing those factors will help you select kits that support clinical needs and long-term practice efficiency.
What Are the Best Practices for Dental Instrument Sterilization and Maintenance?
Proper cleaning, sterilization, and storage protect patients and prolong instrument life. Core practices include:
- Cleaning Procedures: Remove visible debris before sterilization using appropriate detergents and methods.
- Sterilization Methods: Autoclaving is the standard for reliably eliminating pathogens when instruments are prepared correctly.
- Inspection and Storage: Inspect instruments routinely for wear or damage and store them dry and organized to prevent contamination and corrosion.
Consistent adoption of these steps reduces risk and keeps instruments functioning as intended.
What Sterilization Protocols Ensure Safety and Longevity of Dental Instruments?
Robust sterilization protocols combine proper pre-cleaning, validated equipment, and regular monitoring:
- Pre-Cleaning Steps: Rinse and remove gross debris immediately after use to prevent buildup.
- Ultrasonic Cleaning: Use ultrasonic baths to dislodge fine contaminants before sterilization cycles.
- Regular Monitoring: Test autoclaves and track cycle records to confirm sterilization efficacy.
Following these protocols protects patients and helps instruments remain serviceable over time.
How Does Proper Maintenance Enhance Instrument Durability and Performance?
Routine maintenance—cleaning, inspection, lubrication where applicable, and timely repair or replacement—keeps instruments sharp and reliable. Well-maintained tools reduce the risk of intraoperative problems and deliver more consistent clinical results.
Investing in preventive care for instruments lowers long-term replacement costs and supports uninterrupted clinical operations.
How Are Ergonomics and Material Innovations Shaping Dental Instruments in 2026?
By 2026, ergonomic engineering and new material technologies are shaping instruments for better clinical performance. Ergonomic handles, optimized balance, and lighter constructions reduce hand strain and improve control during delicate procedures.
Material advances—like higher-grade stainless steels and improved surface treatments—boost longevity and maintain cutting edges longer, even under frequent sterilization cycles.
What Advances in Stainless Steel Alloys Improve Instrument Durability?
Contemporary stainless steel alloys offer improved corrosion resistance and wear properties. Refinements in alloy composition and heat treatment, along with protective surface coatings, make instruments less prone to pitting and dulling—extending their usable life in busy practices.
These material improvements translate to more reliable instruments and fewer unexpected replacements.
How Does Ergonomic Design Benefit Dental Professionals and Patients?
Ergonomic instruments reduce clinician fatigue and improve hand control, which supports more precise, comfortable procedures. For patients, that increased control often leads to smoother appointments and better clinical outcomes.
Prioritizing ergonomics in instrument selection supports staff well-being and enhances the overall patient experience.
Frequently Asked Questions
What are the benefits of using specialized dental instrument kits?
Specialized kits give you a curated set of instruments tailored to the procedures you perform most. They simplify setup, reduce instrument search time, and can be more economical than buying each item separately. In short, kits improve efficiency, consistency, and cost predictability for your practice.
How often should dental instruments be inspected for wear and tear?
Inspect instruments after each use and before sterilization to catch dulling, corrosion, or mechanical damage early. Any instrument showing compromised performance should be repaired or replaced promptly to maintain safety and clinical quality.
What role does ergonomic design play in dental instrument selection?
Ergonomics impacts clinician comfort, precision, and endurance. Instruments designed to fit the hand and reduce strain enable longer, more accurate procedures and lower the risk of repetitive-stress injuries—benefiting both clinicians and patients.
What are the best methods for cleaning dental instruments before sterilization?
Best practice is to rinse instruments immediately after use, then employ ultrasonic cleaning to remove residual debris. Follow with manual inspection and, if needed, gentle brushing before loading instruments into validated sterilization cycles.
How can dental practices ensure compliance with sterilization protocols?
Create clear, written procedures; train and audit staff regularly; use validated sterilization equipment; and keep detailed cycle records. Regular biological and mechanical monitoring of sterilizers helps verify that protocols are effective.
What innovations in dental instruments are expected in the coming years?
Expect continued advances in materials and ergonomics, plus increased integration of smart features—sensors for feedback, wear indicators, and improved coating technologies to resist corrosion. These innovations will aim to boost performance, safety, and instrument lifespan.
Conclusion
Knowing your instruments—and how to care for them—is fundamental to delivering consistent, high-quality dental care in 2026. Thoughtfully chosen instrument kits, disciplined sterilization practices, and investments in ergonomic and material improvements all contribute to safer, more efficient clinical workflows. Browse our complete range of dental instruments to equip your practice with tools built for reliability and performance.